Whether breastfeeding or not, pumping becomes a necessity for many new moms. But it doesn’t have to, well, suck. Here, we break down the whens, whys, and hows, including how long you should pump in order to make the breast (sorry) of the situation.
How Long Should I Pump? All Your Questions Answered
Why Pump?
There are a variety of reasons why a mom might decide to pump. If you’re away from your baby for any amount of time, whether you’re returning to work or simply running errands, you’ll need to have some breast milk on hand (if you’re not using formula). Also, if your baby is having trouble latching onto your breast, you may need to start pumping as an alternative feeding method.
Plus, it’s a good way to up your milk supply. Dr. Huma Farid of of Boston's Beth Israel Deaconess Medical Center says a mom can pump after every breastfeeding session to increase her supply, adding that keeping track of your baby’s wet diapers and bowel movements is a good way to know if you’re producing an adequate amount of breast milk. On the flip side, if you’re producing a lot of breast milk and feeling engorged, you can start pumping to help relieve the pressure, says Dr. Natasha K. Sriraman, associate professor of pediatrics at Eastern Virginia Medical School in Norfolk, Virginia.
When Should You Pump?
If you’re planning to exclusively pump, start right away. “An early start is important for a strong milk supply so put your baby to breast or start pumping one to three hours after your baby is born,” explains nurse and lactation expert Helen Anderson.
That’s because your body is revved up and ready to go. “Your hormones have been preparing your breasts to make milk since early in your pregnancy. High levels of the hormone progesterone keep a lid on prolactin, but when your baby is born progesterone levels drop off, signaling your breasts to start making milk,” Anderson says. “Putting your baby to breast or using your pump stimulates your nipple and areola nerves, signaling the pituitary gland in the brain to release two hormones, prolactin and oxytocin. Prolactin causes your alveoli to take nutrients (proteins and sugars) from your blood supply and turn them into breast milk. Oxytocin causes the cells around the alveoli to contract and eject your milk down the milk ducts, causing your milk to ‘let down’ or eject.”
If you have a healthy, full-term baby and are breastfeeding successfully, you can wait a few weeks to start pumping. Anderson recommends starting two to three weeks before you plan to return to work—though you may want to start earlier if you want your infant to practice taking a bottle.
How Long Should You Pump?
For moms who are exclusively pumping, Dr. Farid says they will need to pump every two to three hours (even at night) for about 15 to 25 minutes in order to completely empty the breast. “Each lactating mother is slightly different and may have more or less breast milk and may empty the breast faster or slower, so these are approximate times. I recommend watching and waiting until the last few drops of breast milk have been expressed and then pumping for approximately another two minutes to ensure that the breast is completely empty.”
Anderson, who invented the Milkies Milk Saver, a breast milk collection device, explains that this time interval mimics your baby’s feeding habits. “Most babies eat every two to three hours, so try to pump at those intervals to keep your supply strong. These intervals apply to the hours you spend at work too. Try and take two to three pumping breaks in an eight-hour shift to replace the milk your baby is eating and keep your milk supply up.”
And remember, you have those rights. According to the Break Time for Nursing Mothers law, employers are required to provide break time for women to express milk, along with a private space (that is not a bathroom) where they can pump.
Some experts like Laene Keith, a lactation consultant at Health First’s Cape Canaveral Hospital, recommend that moms aim for a minimum of eight pumpings in 24 hours, since you might not be able to space out the sessions evenly throughout the day. “A mother who is exclusively pumping for her newborn will observe her milk increasing on a daily basis and should be nearing 750mL (25 ounces) of pumped milk by day 10,” she adds.
If you’re currently breastfeeding, Anderson suggests pumping between feedings. “For example, if your baby feeds around 8 a.m. then naps until 10 a.m., pump around 9 a.m. By adding in this pumping session every day, or even every other day, you will have a good stash of milk ready when you return to work. Almost every mom worries about having enough milk stored when she returns to work, so start early if you need peace of mind.” If your baby is sleeping through the night or in four- to six-hour stretches, you might want to add in a pumping session then as well, she says.
Dr. Sriraman counsels nursing moms who are starting to pump to do so in the early morning hours, because you tend to make the most milk between 2 to 5 a.m. And like Anderson, she also encourages moms to start pumping once a day as they begin to build up their milk supply.
Keep in mind that pumping breast milk is not as efficient as breastfeeding. “Most mothers will produce anywhere from one to four ounces per pumping session (not per breast) and this is completely normal” Dr. Farid explains. “I advise women not to stress about the ounces of breast milk produced. There are day-to-day variations in how much breast milk women can produce, just as there are day-to-day variations in how much the baby will drink.”
Tips For Effective Pumping
First, start with a good pump. Anderson says that an electric double pump (which pumps both breasts at the same time) allows you to get more milk in a shorter amount of time.
The funnel part of the pump that sits on your breast is known as the flange, and it needs to fit your body, Anderson says. “If there is a bit of space around the nipple and it moves easily as you pump, your flange is probably correctly sized. If there is pain or rubbing, see a lactation consultant or call the pump company and get another size flange,” she says.
She also recommends wearing a hands-free pumping bra to keep the flanges in place. Plus your arms won’t get tired from holding the pump and it’ll be easier to maneuver if you need to adjust the suction. (D.I.Y. tip: Make one out of an old sports bra by cutting holes in the cups where your pump sits.)
To keep your milk supply strong and shorten pumping time, Anderson suggests using breast compression while you pump to help empty your breasts: Use your hands to place gentle pressure on each breast, moving your milk from the back of your breast toward the nipple. Dr. Farid also recommends placing warm compresses on the breasts to encourage milk flow.
Lastly, Anderson says that “pumping is a mental exercise and stress can keep your milk from letting down. If you’re at work, take a few minutes to switch gears or have a picture of your baby to remind you of being with her. Relaxing will help your milk flow better and make pumping less of a chore.”
Doctor-recommended Breast Pumps To Try:
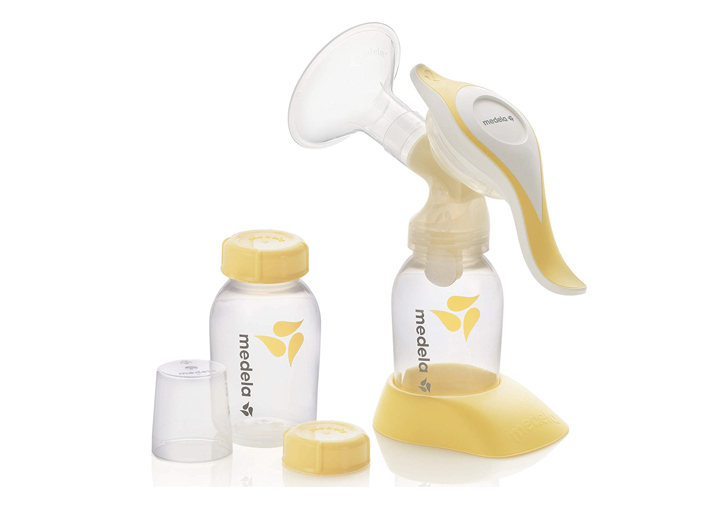
Medela Manual Breast Pump
For moms who are breastfeeding but whose baby doesn’t completely empty the breast, Dr. Farid recommends the Medela Harmony Breast Pump, a manual pump that is designed for occasional use.
Haakaa 5oz Breast Pump
Another manual breast pump, Haakaa is most useful immediately after breastfeeding.
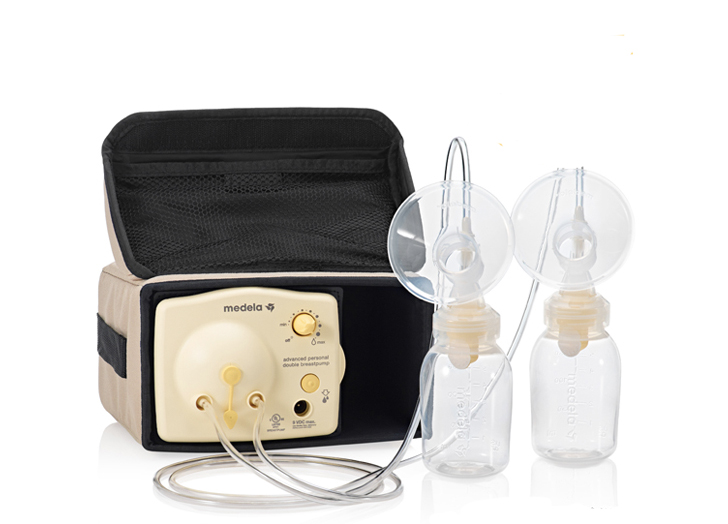
Medela Advanced Personal Double Breast Pump Starter Set
Dr. Farid says that many hospitals have the hospital-grade version of Medela’s electric double breast pump on their labor and delivery and postpartum floors.

Spectra S1 Plus Electric Breast Pump
Owned and operated by moms and registered nurses, Spectra is a newer brand offering electric breast pumps that aim to mimic natural nursing.
Buy it ($200)

Motif Luna Breast Pump
The Motif Luna Breast Pump matches your baby’s natural nursing pattern.

Lansinoh Smartpump Double Electric Breast Pump
Lansinoh Smartpump Double Electric Breast Pump connects to your phone so you can easily track how much you're pumping.